AROUND 300 patients undergo surgery at Salisbury District Hospital every week with operations taking place across 17 theatres (10 main theatres, six Day Surgery Unit and one obstetric theatre).
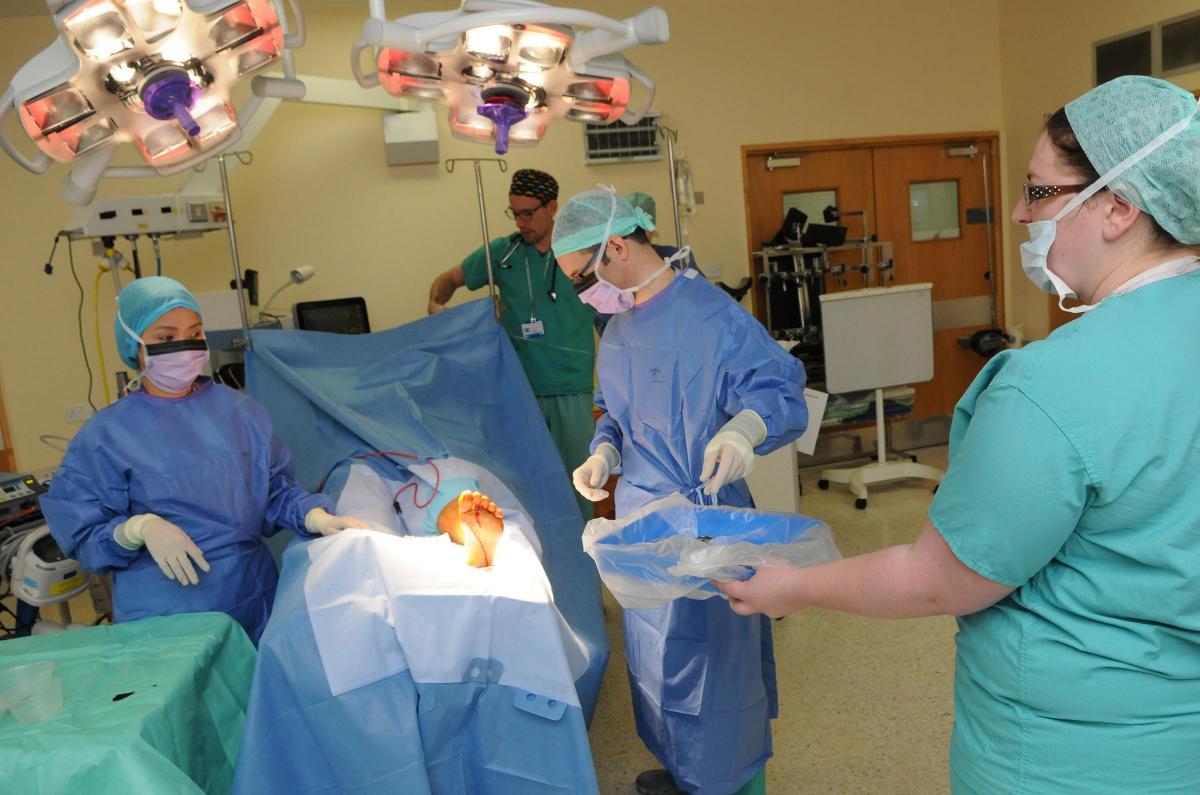
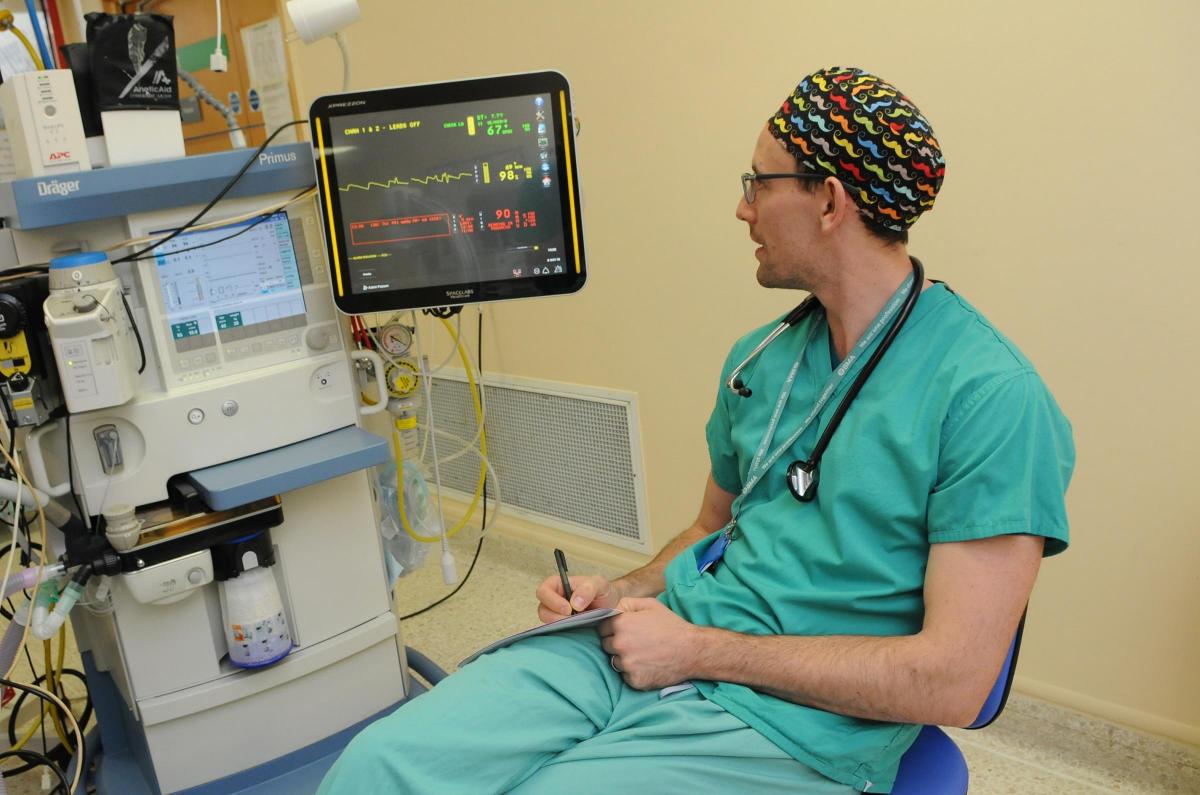
A patient’s operation and aftercare is looked after by a team of around 160 people comprising surgeons, anaesthetists, scrub nurses, recovery nurses, ward nurses, operation theatre practitioners, nursing assistants, cleaners, orderlies and reception staff.
There are two main theatres that run 24/7 and these cover all emergency cases including trauma and obstetrics.
All other theatres principally run 8am-5.30pm, Monday-Friday.
Day surgery (70 staff) generally covers areas such as orthopaedics, plastics, gynaecology, urology, ophthalmology, general surgery and oral surgery.
Much of it is keyhole surgery with some of the most common operations being hernia repairs and arthroscopy (treating joint problems).
“We also do a lot of dental extractions such as the removal of wisdom teeth,” says Bernie Dunn, the day surgery senior sister. Most of the cataract surgery happens here while we also do spinal injections to help mobility and back issues, and we work a lot with the breast care team.”
Patients either come in and go home the same day or stay overnight on the ward before being discharged.
Both adults and children are cared for in the unit with paediatric nurses among staff.
“For children, it is often tonsils, dental surgery or grommet surgery which helps hearing,” Bernie says.
In main theatres (90 staff), operations are generally more complex with patients having either arrived via a ward in the hospital or through the surgical admissions lounge. This is often because of their complex medical history or because of their requirement for urgent or emergency surgery. These patients generally require a longer overall recovery period within the hospital and therefore following surgery they will go back to their ward as an inpatient.
The two departments work closely together with many staff rotating between main theatres and day surgery.
Theatre manager Gary Dawson who oversees both departments said: “One of the challenging factors for the Trust is the way in which healthcare is evolving. There is a real push to look at how we do things differently, in a way which maintains quality of care and benefits patients.
“For example, we are looking at every operation to see whether it needs to stay as main theatre work, if it historically has been, with the idea of moving it into a day surgery setting. With the impact a long stay in hospital can have on a patient’s wellbeing and medical fitness, it is sometimes much better for the patient to recover in their own home.”
In day surgery there are 32 trolleys with some people coming in the morning and in afternoon.
“We treat everybody individually,” Bernie says. “Some people are quite anxious.
“Our nurses spend time with patients, talking to them about their operations and listening to their concerns.
“We try and make it as nice as we possibly can.
“Nursing assistants will bring the patient into the operating theatre and sit with them while nurses will look after them as they recover and the same nurse will discharge them once they are ready.”
Bernie, who has worked at the hospital for 25 years first began as a registered nurse in main theatres before going onto work as a recovery nurse and then into the day surgery unit where she became ward sister and then senior nurse.
“Friendliness and a team working ethos is key for anyone thinking about working in day surgery or main theatres, as is the desire to want to make a difference,” she said.
“On the wards, nurses and nursing assistants are looking after a different group of patients every single day so you are meeting new people all the time.
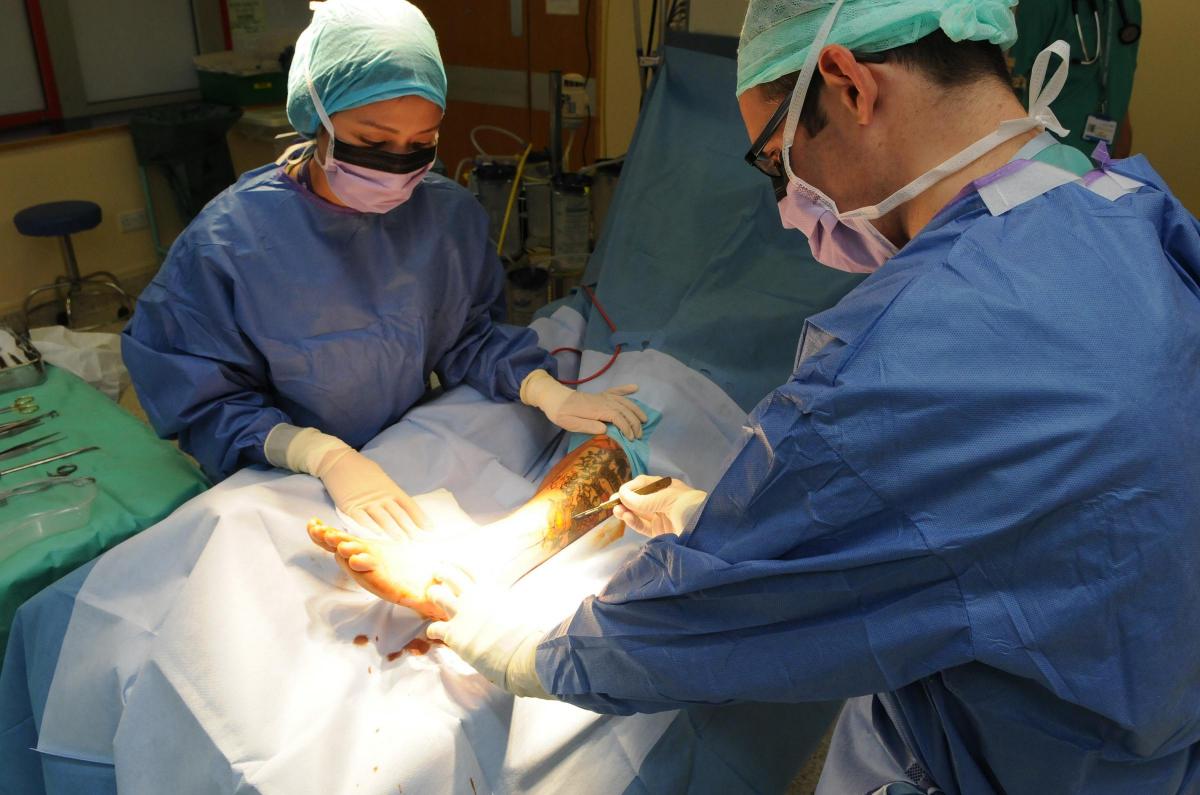
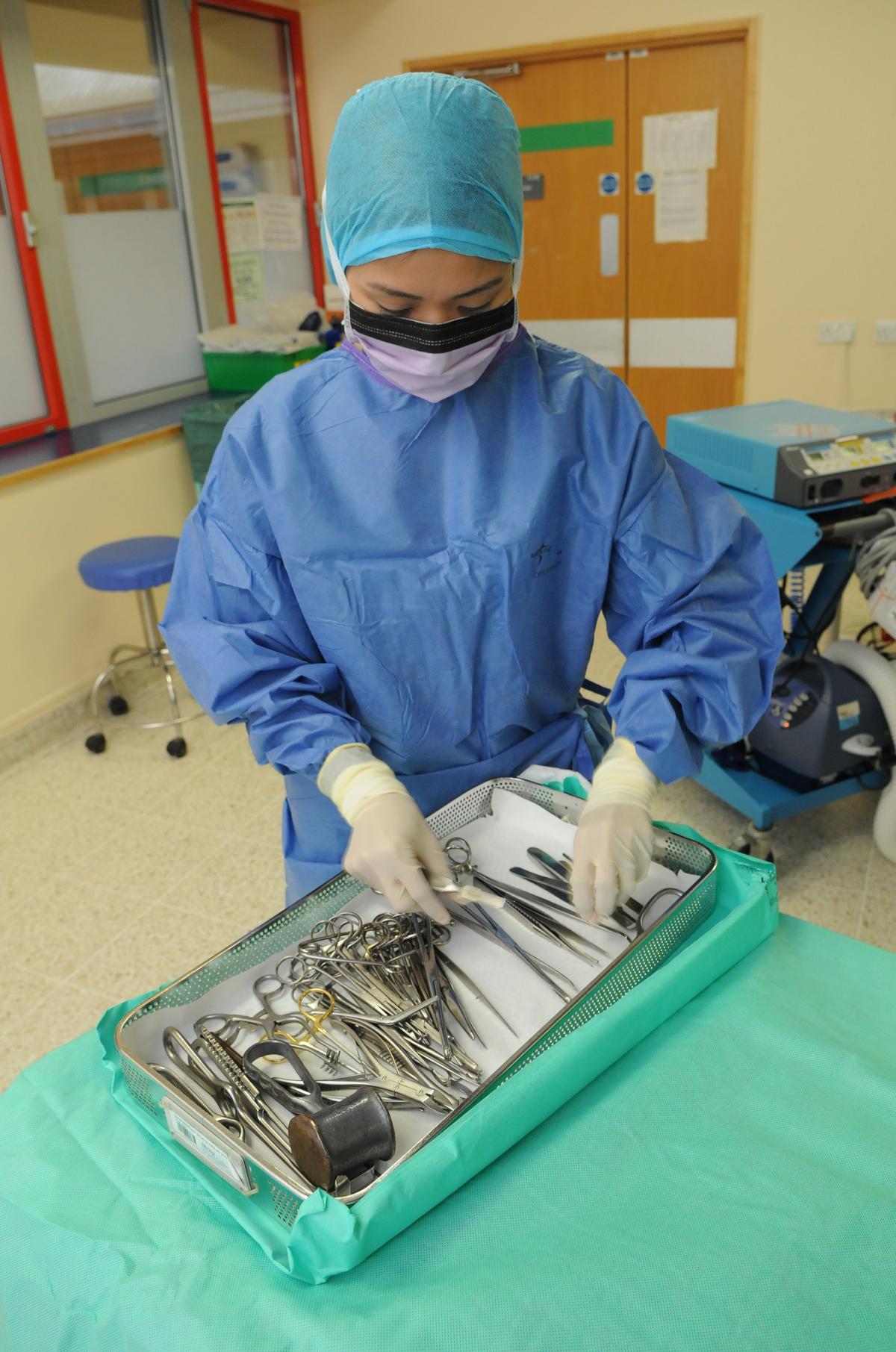
“In theatres, nursing roles are highly skilled, working with instruments during operations. “It’s very interesting and is a different way of looking after patients which is quite challenging.
“It’s a good area where you can improve your skills and increase your career prospects.
“I love the variety of the work and we have a really good team. We do the best for our patients and we enjoy each new day.”
Gary who first trained as a radiographer at the hospital in 1996 has most recently worked in programme management and theatre transformation.
He said: “Resourcefulness, the ability to adapt to many different situations and pulling together as a team are all really important skills to have working here.”





Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereLast Updated:
Report this comment Cancel